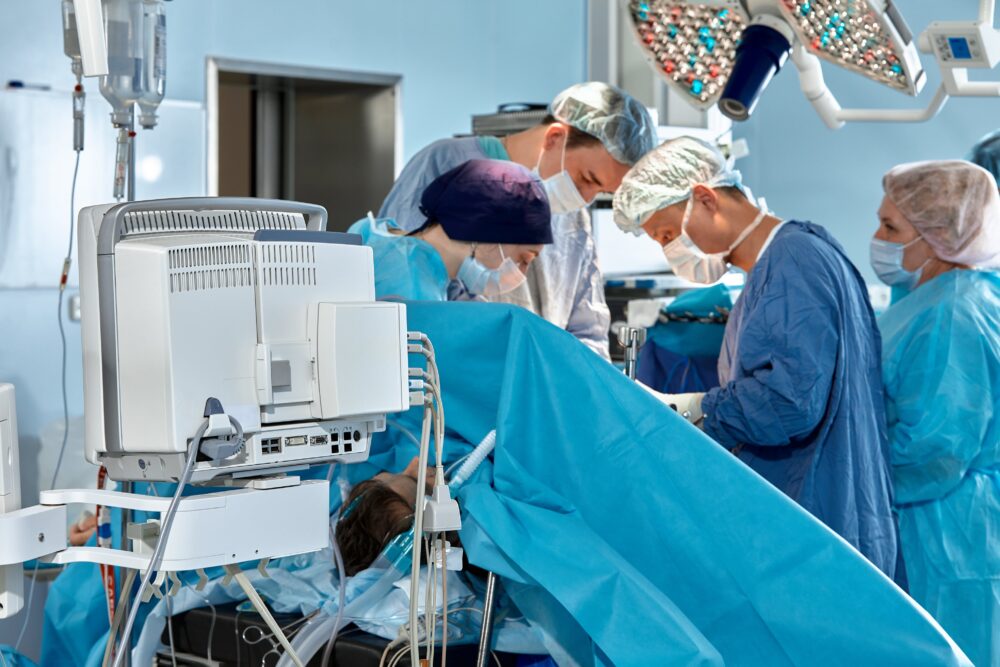
Today hypnosis is widely used by psychotherapists, psychologists and other clinicians in Western medicine to treat a range of conditions. But there are those in the medical field who believe its full potential has yet to be fulfilled and that it could be employed more widely in the operating theater instead of general anesthesia.
Looking back over the centuries and across different cultures, the use of hypnosis, mesmerism and trance-like states in medicine is well documented. Hypnosis has been used for pain relief since the 1840s when Scottish surgeon James Esdaile employed his own form of mesmerism with success during major operations, according to Dr. Carol Ginandes, clinical health psychologist and Ph.D. assistant professor of psychology in the department of psychiatry at Harvard Medical School.
However, with the discovery of ether and chloroform later in the decade, it was side-lined as a medical tool. Dr. Ginandes said:
“Hypnosis is not integrated into the medical milieu and yet there are many studies that show it can be used in lots of situations adjunctively to great advantage. It could be employed in some situations, with certain individuals, who have the capacity and have been prepared in the right way, instead of general anesthesia. The advantages are numerous: general anesthesia is a tremendous stressor on the human body, and it can destabilize the many dynamic variables of homeostasis in the surgery itself.”
Using Hypnosis During “Awake” Brain Surgery
In 2018, Prof Alessandro Frati, Associate Professor of Neurosurgery at the Sapienza University of Rome and Consultant Neurosurgeon at Sant’Andrea University Hospital, undertook a study trialing the use of hypnosis during “awake” brain surgery. All six of his hypnotized patients reported significantly less pain and discomfort than would normally be expected during and after the surgery. He explained:
“Hypnosis gave us the opportunity to test all the neurological functions of the patient during surgery with the patient completely unaware of being operated on, but differently convinced that he was in a different situation, more pleasant and less stressful.”
Through hypnosis, the patients achieved a transient dissociation state before the operation. He added:
“Hypnosis-aided resection of an intrinsic brain tumor located in eloquent areas is safe and effective. It decreases the incidence of intraoperative pain and complications and postpones refractoriness to intraoperative neurophysiologic monitoring and neuropsychological testing.”
Psychiatrist Prof Henriette Walter, a retired professor from Vienna Medical University, runs training courses in medical hypnosis. She said:
“Hypnosis can be very effective in a range of medical areas. It could be used to replace anesthesia in minor surgery, such as skin surgery, and in dentistry. It can be very helpful if you are pregnant or have an allergy to pain medication. I do think we should educate our medical doctors more on the possible uses of hypnosis.”
Dispelling the Myths
Dr. Ginandes, who has explored the use of hypnosis throughout her career, has found it useful as a tool to relieve pain and ameliorate healing following surgery. She prepares her patients hypnotically by devising audio programs for them to listen in before the procedure.
Her own research studies have shown bone fracture and elective breast reduction surgery patients who have been hypnotized in addition to receiving standard medical treatment have healed more quickly than those receiving the standard treatment alone. She said:
“There are many studies that have shown hypnosis doesn’t just relieve pain but can ameliorate and speed up recovery and in the surgery itself it can stabilize blood flow and dynamic variables. As an adjunct or substitute for general anesthesia, hypnosis has tremendous value.”

The barrier to wider use, she believes, is prejudice and lack of knowledge:
“Unfortunately, hypnosis has always been associated with the trope of the guy in the black cape waving a pendulum in front of the person who is generally pictured as a young woman. The implication is that hypnosis is some form of control—and a malevolent one at that. In fact, that is very far from the truth. It empowers a patient rather than resulting in them being in less control.”
We All Have Access to It
Another common misconception is that patients less susceptible to hypnosis might “wake up” during the procedure. Dr. Ginandes said:
“Hypnosis before surgery requires careful preparation and practice. It is not like a light switch, which either works or doesn’t work, it can help to a greater or lesser degree.”
It is an old-fashioned notion that some people can’t be hypnotized, she suggested.
“Hypnosis is a state of absorptive, focused awareness that chances are all of us naturally drift in and out during the course of our day. It is different from sleep or from a kind of linear waking awareness and it is a state that appears to be wired into our neurophysiology. We all have access to it with proper instruction.”