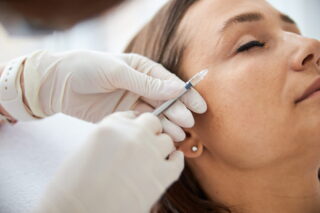
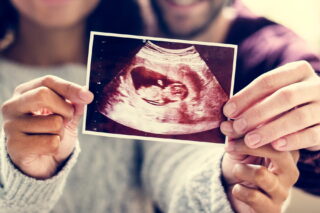
Artificial Intelligence (AI) radiology solutions for adults are developing at pace, but according to experts at this year’s ECR Overture, when it comes to pediatrics there is still some way to go.
Prof. Dr. Erich Sorantin, University Clinic for Radiology at the Medical University of Graz, Austria, suggested many areas of radiology could be enhanced by AI. But according to him, we are still far from the futuristic, science fiction solutions some have predicted in the past. He explained:
“If you look at Star Wars, they had something like a CT or mini MRI at the beginning, but by the end they had one very nice gadget to diagnose almost everything—and that is where we should go.”
Prof. Loukas Astrakas, a doctor at the University of Ioannina, said AI could eventually be used in pediatric radiology, but only alongside humans. He said:
“There are many different tasks that can be performed with AI, from the detection of diseases, such as breast, brain and prostate cancer, to chest radiograph interpretation.”
The “Black Box Problem”
He also cited many problems:
“AI algorithms can overfit or underfit. In overfitting you train it so much that it becomes very good in its data set but cannot generalize for others. In underfitting you do not train them efficiently and the algorithms cannot extract data.”
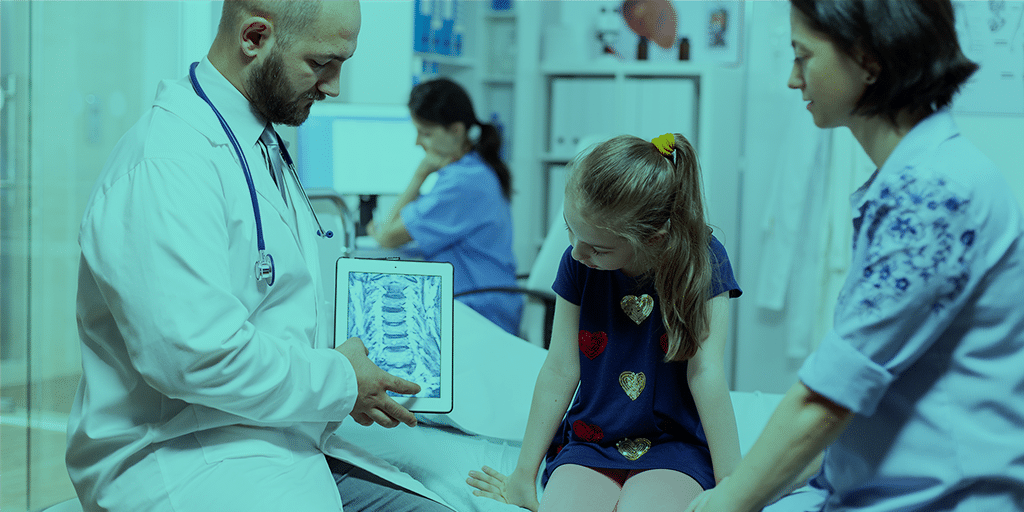
He added:
“Then, there is the ‘black box problem’—will people accept a diagnosis if the doctor cannot explain how it was arrived at? And also the issue of medical-legal responsibility—who is responsible if something goes wrong with an AI diagnosis?”
The best approach, he stressed, is to combine AI with the human brain in pediatric radiology because they excel in different domains.
“Human intelligence is able to imagine, anticipate, feel and judge changing situations. AI is better at low level, routine tasks that are repetitive and take place within closed systems. Adopting AI will benefit the careers of pediatric radiologists, but most importantly the lives of their patients.”
Lack of Research
Radiologist Steven Schalekamp, of the Diagnostic Image Analysis Group in the Netherlands, said there were now 57 CE-certified AI products but none specifically designed for children. He explained:
“There is a great discrepancy in products that are available for adults and for children. The problems are that there is much less research into pediatrics and a lack of data to train systems: an AI system using adult data might not be able to use that to assess a child. There is a big difference in the thorax of a child and an adult; children’s growing chests are constantly changing and the system has to look for different abnormalities.”
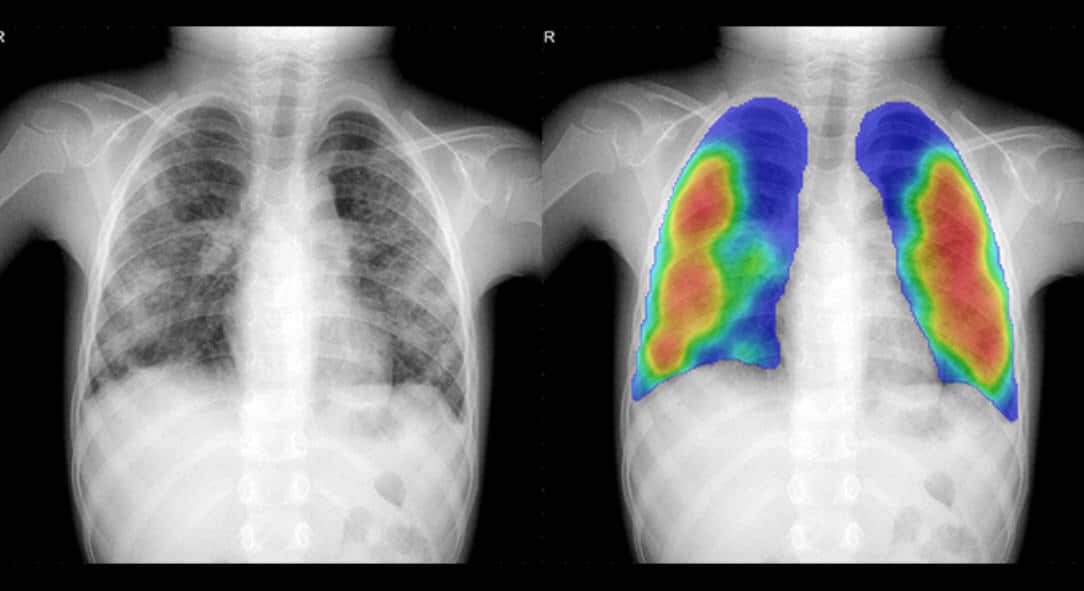
There is only currently one solution available that is also applicable to children. This is the CAD4TB by Delft Imaging, a software product able to detect TB in chest radiographs. There is an emerging application for pneumonia in children, called CAD4Kids, but at the moment further development is required.
AI could be useful in the assessment of neonatal radiographs and the grading of infantile respiratory distress syndrome (IRDS) in premature babies. Steven Schalekamp observed:
“Another area that has been getting a lot of attention in recent years is the use of AI for the tracking of cystic fibrosis in chest CT scans. I think it is important now that vendors try to develop specific products for the pediatric population. But more research is needed. The first step is to transfer the learning of current AI systems and retrain them on pediatric data.”