This summer, MedicalExpo e-magazine is highlighting ten of its most popular articles published in 2023—an opportunity to review the cutting-edge innovations and digital technology that have made an impact in several healthcare sectors this year. Here is article #1. It was first published on January 23, 2023.
The field of nanorobotics in medicine is as complex and challenging as might be expected, but across the world researchers are making huge strides with pioneering technologies. For the treatment of cancer, the hope is to be able to deliver precise doses of effective drugs directly to tumors, thereby minimizing the toxic effects on other parts of the body. In neurology, the expectation is that one day tiny “machines” will be able to clear blockages, dissolve blood clots and administer microdoses of medicine within the brain itself.
Deep brain stimulation, where treatments are carried out via external devices that transmit electrical pulses to the brain, may be replaced by internal robot stimulation. And there is hope that sending nanoelectronic biosensors into the body might assist the diagnosis of disease and other health conditions.
According to Dr. Daniel Ahmed, Professor of Acoustic Robotics for Life Sciences and Healthcare at the Acoustic Robotics Systems Lab (ARSL) at ETH Zürich, technologies are developing at pace. They could change the face of cancer treatment and neurological surgical intervention. He said:
“The idea is for medical professionals to be able to carry out whole procedures that are non-invasive.
For example, we hope to be able to treat aggressive brain tumors, such as glioblastoma that can be hard to reach, without impacting the rest of the body, and to carry out procedures inside the body using microrobots that could prevent strokes.
The vision is to be able to navigate them within the brain for all sorts of applications, including opening up the blood-brain barrier (BBB).”
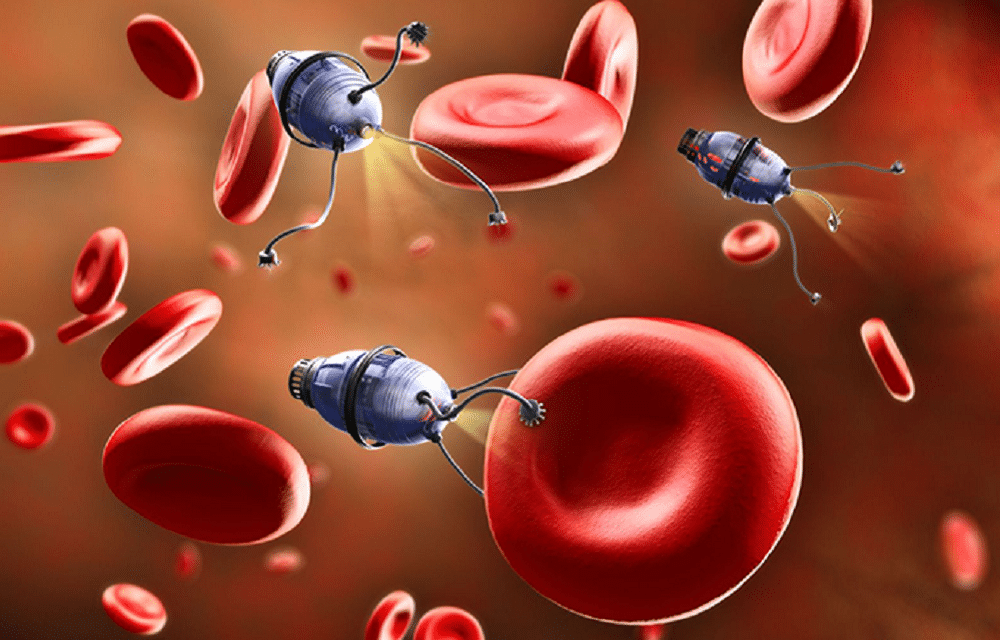
The BBB is an essential immunological feature of the central nervous system. To protect the brain, it blocks microorganisms that might otherwise enter via the bloodstream. He added:
“The hope is to be able to open up the BBB in a very controlled way. If we can do this, then we can start delivering drugs straight to the brain.”
Tiny Travellers
According to Prof. Ahmed, the terms “micro” and “nano” have become interchangeable. Both are used today by scientists, researchers and other experts in smart medicine to describe robots small enough to travel within the human body. The robots themselves may be synthetic devices or completely organic. Equally, they may be created by combining inorganic materials with biological components, such as cells, proteins or DNA.
Many are being designed to work together in “swarms” to achieve their mission. Some are being developed to be inserted into human veins, while others might be ingested. All will need to be able to self-degrade safely after achieving their intended tasks.
Biocompatibility with the human body is essential but the form of the robot also depends on its purpose and how researchers are approaching the challenges of manipulation and propulsion. Prof. Ahmed explained:
“What the robot actually is varies from research project to research project, as well as what type of pill or other treatment you actually want to apply.”
Propulsion Solutions
At the Acoustic Robotics Systems Lab, Prof. Ahmed and his team have worked on six different types of micro and nanorobots. These include an air bubble encased within a polymer shell and an imaging chemical and another—inspired by starfish larvae—that uses tiny hairs to create a vortex for propulsion.
“The biggest challenge is how to propel the robots through the bloodstream to the intended target at this scale, because there is no inertia and the environment is highly viscous. And they cannot complete their function if they are just flowing with the blood.
There is a lot of work going on at the moment where people are using a magnetic field to drag a microrobot, but in in our case we use the acoustic field.
We decided to do this because it is a mature technology. It works in real time and it is already used for imaging in almost every hospital across the world, making it cost effective.”
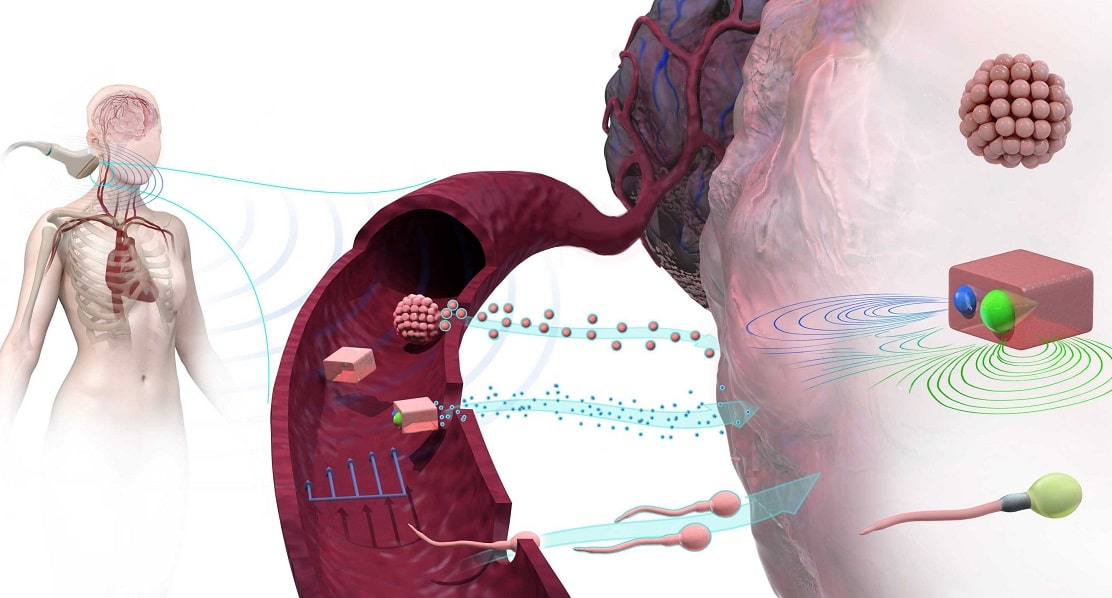
He added:
“The robots we are using for this are basically self-assembled using an ultrasound contrast agent, whereas if you apply a magnetic field, your robot has to be magnetic.”
Researchers from Polytechnique Montréal, Université de Montréal and McGill University have developed nanorobotic agents, composed of more than 100 million flagellated bacteria, to navigate through the bloodstream. The synthesis of a chain of magnetic nanoparticles allows them to move in the direction of a magnetic field, while a sensor measuring oxygen concentration enables them to reach and remain in the tumor’s active regions. Prof. Ahmed suggested:
“Many micro robots are inspired by nature. A good example is how bacteria are propelled by a corkscrew motion or the motion of a flexible sperm cell. And we realized that many of these exploit the wall of the blood vessel.
They go to the wall, where the drag force is the minimum and as a result they can move upstream and can be navigated within the vascular network.”
Smart Choices
Prof. Ahmed and his team are also looking at how the robots might eventually be able to auto-train and navigate themselves using artificial intelligence.
“It is very exciting, but there will be lots of challenges as we move away from the mice we are planning to work with soon and into higher mammalian models.
The regulation becomes much stricter and then when you move into humans there is the question of whether people will accept the technology—but I think they will.
Of course, we will have to study controls and take safety measures but, although I think this will be a disruptive technology, I also feel it’s a very safe technology.”
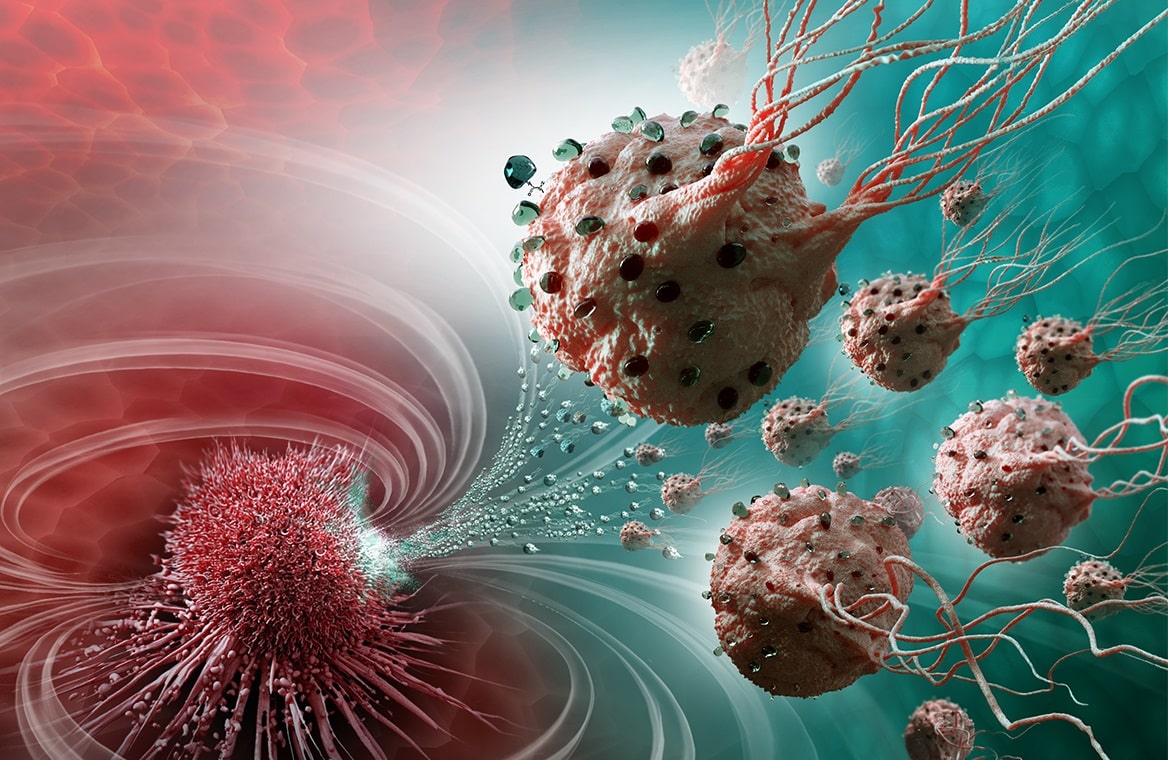
As the different nano and micro robot technologies progress, questions of ethics are likely to be raised. But where robots will disintegrate within the bloodstream after performing, the expectation from those working across the field is that both patients and professionals will be eager for the introduction of any of the technologies that are proven to work.
Prof. Ahmed firmly believes it will not be long before micro and nanorobots are helping to save lives. He said:
“We should be able to develop the technology in five to seven years. And 20 years from now, I really hope it will be available in hospitals across the world.
By then, it should have reached a maturity where the patient makes a decision on whether to go with a nanorobotic option or to go for a more traditional alternative.
But if you consider that alternative might involve cutting into the skull or the serious side effects of cancer treating drugs, then I think patients will choose this. And, hopefully, as our research progresses, we will also be able to look at whether we can use similar technologies in the prevention of diseases such as Alzheimer’s and epilepsy.”