Discovered in 2013, the CRISPR-Cas9 new revolutionary technique of gene editing has been much talked about. Is it a miracle solution to treat genetic diseases? A new way, faster and simpler, to make GMOs? Or a powerful tool to augment humans and create a new, more resistant human kind? With the CRISPR designer babies scandal in November, the scientific community is debating whether to put in place ethical rules and regulations on an international level. We spoke with Richard Sherwood, Assistant Professor of Medicine at Brigham and Women’s Hospital in Harvard Medical School (Boston), about the benefits and drawbacks of this technology. He created InDelphi, an algorithm that can predict CRISPR repair outcomes.
ME e-mag: Can you quickly explain how CRISPR-Cas9 works?
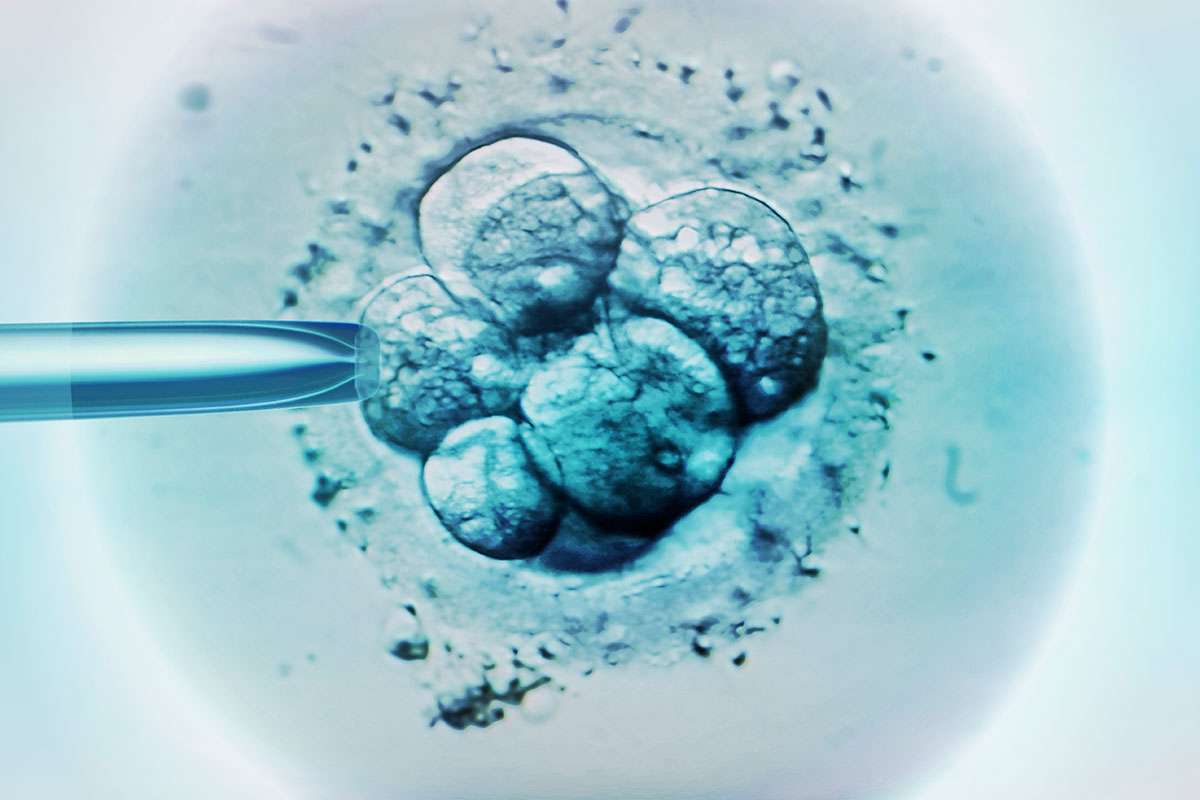
R. Sherwood: CRISPR-Cas9 is a bacterial immune system against viruses. Bacteria have evolved a way to recognize specific DNA sequences and then use the Cas9 enzyme, which is a molecular pair of scissors, to chop that DNA sequence which will basically kill the virus. What researchers have been able to do over 20 years of research is hijack that system so that now just by guiding the Cas9 enzyme to any DNA sequence of your choice in a human cell you can get the Cas9 enzyme to cut that sequence. Then what happens is that the human cell, as opposed to the virus, doesn’t just die, it finds a way to repair that cut. That repair often causes a mutation.
“That’s really the heart of the CRISPR Cas9 field: causing DNA mutations.”
That’s really the heart of the CRISPR Cas9 field: causing DNA mutations. From a research perspective, it’s incredibly useful because many inherited genetic diseases, as well as cancer, are actually caused by DNA mutations. Before CRISPR-Cas9, it was quite difficult to induce those mutations or to recreate those mutations, so it was very hard to study genetic diseases. With CRISPR-Cas9 it made that process way easier and faster.
ME e-mag: Is CRISPR-Cas9 already being used on humans?
R. Sherwood: There’s a lot of excitement right now because there are many genetic diseases out there and CRISPR is a technique to remedy these diseases. But clinical applications will take longer. There are currently clinical trials to use CRISPR-Cas9 in therapies but no approved uses yet. It will probably happen in the next five years. The ability to use this technology on human cells was only discovered six years ago. So it hasn’t been long enough for the first therapies to be developed.

The CRISPR “Designer” Babies
ME e-mag: But in November a Chinese scientist shocked the world when he announced that he had created the first babies genetically edited with CRISPR…
R. Sherwood: That’s called germline gene editing. All of the clinical trials that are currently going on are doing what is called somatic gene editing, where you take an adult patient and try to edit the genes that might carry a genetic disease. This researcher in China claimed that he actually edited the genes of a fertilized egg and made babies (twin sisters) out of that.
“It’s well known that there are a series of potential limitations of CRISPR that can cause what we call “off-target effects”—where basically in addition to breaking what you want to break, it can break something else in your genome.”
It was pretty much universally condemned by the scientific community because, while this is a promising research field, the benefits and drawbacks have not been studied nearly enough to know that this could be something safe to do to a baby. It’s well known that there are a series of potential limitations of CRISPR that can cause what we call “off-target effects”—where basically in addition to breaking what you want to break, it can break something else in your genome. Even if that happens at a very low rate, it’s one thing if you do that on an adult patient and possibly deal with the consequences, and it’s another thing if you do that on a baby. At this point there are no laws but the majority of the community has widely decided that this is not an appropriate application.

The other reason why there is not a lot of enthusiasm for using it on the germline is because we have better techniques. If you know that a genetic disease runs in your family, there are techniques like embryo selection where you can select embryos that you know don’t have that disease gene. So until the research progresses further, there is no reason why CRISPR would be a better approach.
CRISPR and Artificial intelligence
ME e-mag: Could you tell us more about InDelphi?
R. Sherwood: The motivation for what we did is that most people have been using CRISPR to break genes. I often use this analogy: if you have a hammer, the easiest way to use it is to just break something, but you can also use it to chisel and make a sculpture if you use it in the right way. That’s what we were looking at: can we use Cas9 in a more refined way to know what we are doing and in some cases actually be able to fix broken genes?
The actual process we were looking at is about what happens in a cell after the DNA of that cell has been cut with CRISPR. We found out that when a cell has been cut the repair is not random; there are very specific ways that the cell repairs CRISPR’s cuts. So we were able to use machine learning to have a computer program that can predict how this happens. So now what we can do, and that has not been possible before, is when CRISPR gets directed to a site in the genome we can actually predict what sort of mutations will be caused.
“Our algorithm was able to find patterns and one of the really surprising things that came out of this was that there are certain places in the genome where when CRISPR cuts, the cell basically has one dominant way of repairing that break.”
ME e-mag: How does the machine know that? How do you train it?
R. Sherwood: We do this by generating lots and lots of data. We developed an approach where we could target CRISPR to thousands of different sites in the genome and monitor what sorts of mutations it can cause. That was a rich dataset that included hundreds of millions of actual DNA mutations. Using that unprecedented large dataset on the types of mutations caused by CRISPR, then we were able to train the algorithm to look for patterns. It was able to find patterns and one of the really surprising things that came out of this was that there are certain places in the genome where when CRISPR cuts, the cell basically has one dominant way of repairing that break.
It’s like if you break a piece of glass, you expect it to shatter into multiple pieces and you can’t predict what sort of pieces you get. What we were showing is that if you break a piece of glass (at one specific location), it will always break in one particular way.

ME e-mag: How can you be sure the predictions of the machine are correct?
R. Sherwood: In the machine learning field, there are pretty standard ways of testing the accuracy. Generally you train your program on 80 or 90% of your data and then use the remaining 10 or 20% to test how well the algorithm does. Our algorithm was extremely accurate at predicting the repair events. Since then we actually made a whole other set of thousands of broken sites in the genome and found that the algorithm was equally accurate at predicting what happened at those sites.
We only did this on cells in a dish. Before we would ever think about using it therapeutically on patients, we want to test it in animal models and eventually on more clinically relevant settings.
ME e-mag: Why are you so reluctant to test it on patients? What could be the risks for them?
R. Sherwood: We want to be really careful because the main danger is causing unintended mutations. Basically you have a pair of scissors that’s going into the genome and by using your specific guide RNA you can direct this pair of scissors to cut one particular place in the genome. But every once in a while it will make a mistake and cut at a different place in the genome.
“We want to be really careful because the main danger is causing unintended mutations.”
Let’s say you want to use our technique to correct a gene in the liver of a patient. There are over a billion liver cells so we try to correct the gene in a billion liver cells. The off target rate of CRISPR is somewhere around 1%. That still means that there are ten million cells that are going to get some sort of unintended mutations so that’s a very large number. That’s why when you’re working to try to correct genes on such a large number of cells the bar of how accurate you need to be is way higher than what we’ve currently been doing in terms of researching genetic diseases in cells in a dish. We don’t really know what types of damage we can cause—that’s why we need to do much more research before using it on patients.
CRISPR and Cancer
ME e-mag: Is CRISPR the miracle therapy of the future?
R. Sherwood: I think there is a difference between understanding and treating disease. From an understanding perspective, CRISPR really has changed the genetics field and I don’t think it is too much to say it is a revolution. A major use of CRISPR is in genetic research. Previously it was very hard to understand genetic diseases whereas CRISPR has made it much easier. You can actually create the exact mutation that a patient has with either a genetic disease or with cancer. By doing that you can much better understand for example the differences in a patient’s cancer cells compared to the non cancer cells.

For treating disease, there’s not a single CRISPR treatment that is currently approved in the US or in Europe. I think that, to know whether it really is a revolution in treating patients, we still have to wait and see.
“Cancers are a very hard problem because by the time you have cancer you tend to have a billion, sometimes even a trillion of cancer cells in your body. And cancer cells are very good at hiding in the body.”
ME e-mag: Will it be able to cure cancer one day?
R. Sherwood: Certainly there are genetic diseases that could be treated by CRISPR but I think it would be very difficult to use CRISPR to treat cancer. Cancers are a very hard problem because by the time you have cancer you tend to have a billion, sometimes even a trillion cancer cells in your body. And cancer cells are very good at hiding in the body, so even if we found a way to use CRISPR to kill cancer cells, the challenge would be in delivering CRISPR to every cancer cell. It will be a long time before we’re treating cancer with CRISPR.
Augmenting the Human
ME e-mag: What about using CRISPR on healthy people? Biohacker Josiah Zayner pretends he has been using CRISPR on his own DNA. What do you think?
R. Sherwood: Right now, my guess is that the people who claim they’re using CRISPR outside the medical system are not really doing anything helpful. In the medical field we have a very well tested way of determining whether something is useful for patients that’s called clinical trials. I wouldn’t believe things outside clinical trials much.

ME e-mag: Who is able to use CRISPR technology? Is it easy?
R. Sherwood: Yes and that’s one of the reasons why CRISPR is so revolutionary: for scientists it is extremely easy to use. It’s really best done in a lab setting because you have to introduce both the Cas9 enzyme and the guide RNA into your cell. There are very well distributed tools that make that very easy to do in the lab. This pretty much works on every type of animal or plant. Outside of a lab, I don’t know what sort of people are trying to do some experiments but certainly CRISPR is accessible to any scientist. You can actually buy all the tools you need, including the Cas9 protein itself, that someone else has purified, from medical companies.
ME e-mag: What about the transhumanist perspective of using CRISPR to create augmented humans?
R. Sherwood: In the long term, yes I think it could be used to augment humans because it’s a technology that can change genes. But we’ve been using it for a very short amount of time, and as I said we’ve also seen that it can have unintended consequences. We are still at such early stages of research that the thought of using it for something that is not correcting a genetic disease is to me very premature because we don’t understand the long-term effects. Even in mice or animals we really don’t understand what might happen years after getting the CRISPR therapy.
“In the long term, yes I think it could be used to augment humans because it’s a technology that can change genes.”
There are a couple examples of cases where people have started to think about how we might use CRISPR on healthy patients to prevent diseases. There’s one case that was done in animal studies where it is known that patients who have a broken PCSK9 gene have way lower cholesterol. So they’re less likely to get heart attacks. There’s actually already a drug on the market that kind of soaks up the PCSK9 protein from the blood and lowers people’s cholesterol. That’s already a clinically approved drug but scientists now are starting to think instead of trying to get rid of the PCSK9 protein, what about breaking the PCSK9 gene and then you’ll never ever produce the PCSK9 protein. The research on mice has shown that these mice have lower cholesterol levels and are less likely to suffer from heart disease.
The interesting thing here is that this is not about taking mice with a genetic disease; this is taking normal healthy mice and lowering their risks of getting heart disease. In humans, something around 30% of all people die of heart disease. So if we could find ways of taking healthy people and making them less likely to have a heart attack that would be a very big deal. But there still might be other consequences or side effects that we don’t know right now.
Ethical Regulations
ME e-mag: Do we need to create international ethical laws to avoid other CRISPR babies?
R. Sherwood: That’s certainly becoming a more important issue. The Chinese scientist who claimed he made the CRISPR babies announced that at the International Summit on Human Genome editing. It was a gathering that was supposed to talk about the ethics and implications of CRISPR gene editing therapy. At that same conference, there were scientists who got together and talked more seriously about what sorts of rules and regulations should be put in place to guide the scientific community.

But I think that right now there are no internationally binding rules on what can and can’t be done—certainly here in the USA. If we want to do research on patients, we have to go through a local ethics board that will determine what research is okay. People have talked about instituting a moratorium or a ban on germline gene editing (using CRISPR in fertilized egg) although as far as I know there is actually no legal ban in place in any country. It’s all just up to the local ethics boards. For me, as I work in a hospital, I have to obey these ethics groups. However, for people who are able to do some sort of research outside a hospital or an academic institution, right now there are no legal rules that would prevent them.
“I think the right approach is getting as many people to be knowledgeable on this subject as the technology continues to evolve. It’s not only scientists, doctors or politicians who should have a say. If it was safe enough, would we want to use it as a society?”
There are different opinions on whether there should be. In my opinion, the problem with developing laws is that laws tend to last for long periods of time and sometimes they don’t keep up with how fast science is moving. While this research seems incredibly unethical now, we don’t know what will happen in ten years and it’s very hard to overturn a law. So I think the right approach is having gatherings of scientists, doctors, concerned citizens, getting as many people to be knowledgeable on this subject as the technology continues to evolve. It’s not only scientists, doctors or politicians who should have a say. If it was safe enough, would we want to use it as a society?
ME e-mag: Do you think that with CRISPR we will create a new human kind?
R. Sherwood: In the short term, I would say the answer is no. Many exciting discoveries in medicine have emerged in the last 25 years but it really takes decades for them to start making a big impact on healthcare. One example is using the immune system to fight cancers. That idea emerged in the last 10 to 20 years and only now is there the first immunotherapy on the market—that has had some miracle cures. However it still only works on a fraction of cancer patients, and we don’t know why. So there’s still a long way to go for this revolutionary discovery to become routine. For CRISPR it’s the same thing. We could look at a hundred year horizon I think, then it can have implications and we might be having this discussion again…
>>>> Also read our previous article CRISPR-Cas9, A Troubling Genetic Revolution.